Website content extracted from: Diabetes: 12 warning signs that appear on your skin (aad.org)
Diabetes can affect many parts of your body, including your skin. When diabetes affects the skin, it’s often a sign that your blood sugar (glucose) levels are too high. This could mean that:
If you notice any of the following warning signs on your skin, it’s time to talk with your doctor.
1. Yellow, reddish, or brown patches on your skin
Necrobiosis Lipoidica
This skin condition often begins as small raised solid bumps that look like pimples. As it progresses, these bumps turn into patches of swollen and hard skin. The patches can be yellow, reddish, or brown.
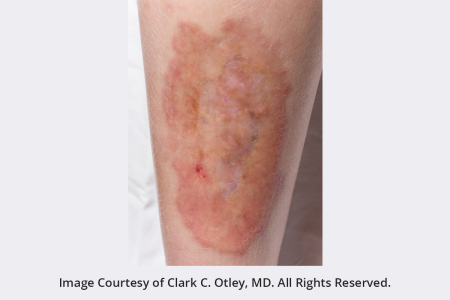
You may also notice:
The medical name for this condition is necrobiosis lipodica.
Take action
2. Darker area of skin that feels like velvet
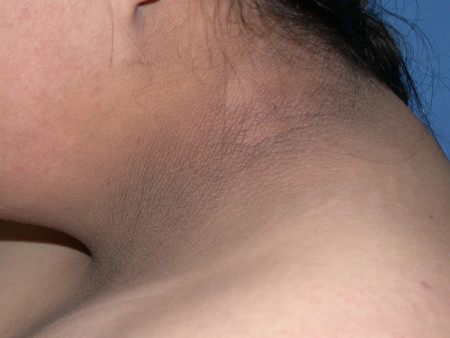
A dark patch (or band) of velvety skin on the back of your neck, armpit, groin, or elsewhere could mean that you have too much insulin in your blood. This is often a sign of prediabetes. The medical name for this skin condition is acanthosis nigricans.
Acanthosis Nigricans (AN)
Often causing darker skin in the creases of the neck, AN may be the first sign that someone has diabetes.
Take action
3. Hard, thickening skin
When this develops on the fingers, toes, or both, the medical name for this condition is digital sclerosis.
On the hands, you’ll notice tight, waxy skin on the backs of your hands. The fingers can become stiff and difficult to move. If diabetes has been poorly controlled for years, it can feel like you have pebbles in your fingertips.
Take action
4. Blisters
It’s rare, but people with diabetes can see blisters suddenly appear on their skin. You may see a large blister, a group of blisters, or both. The blisters tend to form on the hands, feet, legs, or forearms and look like the blisters that appear after a serious burn. Unlike the blisters that develop after a burn, these blisters are not painful.
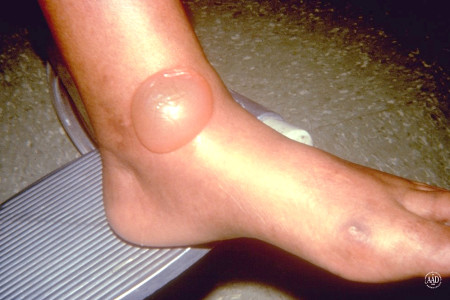
Blisters
Large blisters like this one can form on the skin of people who have diabetes.
The medical name for this condition is bullosis diabetricorum. Sometimes, it’s called diabetic bullae.
Take action
5. Skin infections
People who have diabetes tend to get skin infections. If you have a skin infection, you’ll notice one or more of the following:
A skin infection can occur on any area of your body, including between your toes, around one or more of your nails, and on your scalp.
Skin infections
Has it been a year or longer since your last period, and do you get several yeast infections each year? It’s possible that you have diabetes or pre-diabetes.

Take action
6. Open sores and wounds
Having high blood sugar (glucose) for a long time can lead to poor circulation and nerve damage. You may have developed these if you’ve had uncontrolled (or poorly controlled) diabetes for a long time.
Poor circulation and nerve damage can make it hard for your body to heal wounds. This is especially true on the feet. These open wounds are called diabetic ulcers.
Diabetes and feet
If you have diabetes, you should check your feet every day for sores and open wounds.
Take action
7. Shin spots
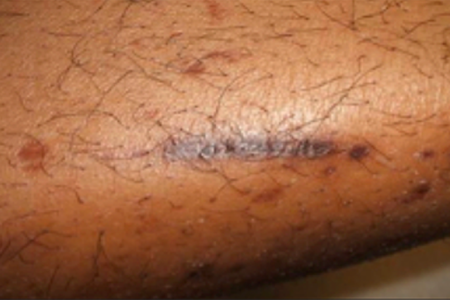
This skin condition causes spots (and sometimes lines) that create a barely noticeable depression in the skin. It’s common in people who have diabetes. The medical name is diabetic dermopathy. It usually forms on the shins. In rare cases, you’ll see it on the arms, thighs, trunk, or other areas of the body.
Shin spots
Diabetic dermopathy: This 55-year-old man has had diabetes for many years.
The spots are often brown and cause no symptoms. For these reasons, many people mistake them for age spots. Unlike age spots, these spots and lines usually start to fade after 18 to 24 months. Diabetic dermopathy can also stay on the skin indefinitely.
Take action
8. Outbreak of small, reddish-yellow bumps
When these bumps appear, they often look like pimples. Unlike pimples, they soon develop a yellowish color. You’ll usually find these bumps on the buttocks, thighs, crooks of the elbows, or backs of the knees. They can form anywhere though.
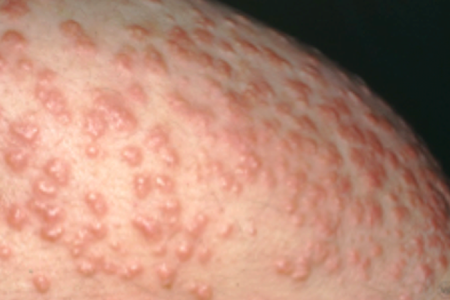
Eruptive-xanthomatosis
These bumps appear suddenly and clear promptly when diabetes is well-controlled.
When these bumps appear, they often look like pimples. Unlike pimples, they soon develop a yellowish color. You’ll usually find these bumps on the buttocks, thighs, crooks of the elbows, or backs of the knees. They can form anywhere though. No matter where they form, they are usually tender and itchy. The medical name for this skin condition is eruptive xanthomatosis.
Take action
9. Red or skin-colored raised bumps
Whether this skin condition is associated with diabetes is controversial. We know that most people who have granuloma annulare do not have diabetes. Several studies, however, have found this skin condition in patients who have diabetes. One such study found that people with diabetes were most likely to have granuloma annulare over large areas of skin and that the bumps came and went. Another study concluded that people who have granuloma annulare that comes and goes should be tested for diabetes.
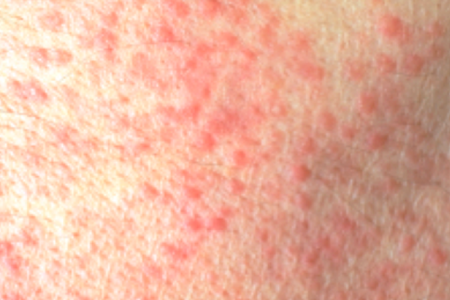
Granuloma annulare
This skin condition causes bumps and patches that may be skin-colored, red, pink, or bluish purple.
Take action
10. Extremely, dry itchy skin
Dry, itchy skin
If you have diabetes, you’re more likely to have dry skin. High blood sugar (glucose) can cause this. If you have a skin infection or poor circulation, these could also contribute to dry, itchy skin.
Take action
11. Yellowish scaly patches on and around your eyelids
These develop when you have high fat levels in your blood. It can also be a sign that your diabetes is poorly controlled. The medical name for this condition is xanthelasma.
Take action
12. Skin tags
Many people have skin tags—skin growths that hang from a stalk. While harmless, having numerous skin tags may be a sign that you have too much insulin in your blood or type 2 diabetes.
Skin tags
These growths are most common on the eyelids, neck, armpit, and groin.
Take action
When to see a dermatologist
Diabetes can cause many other skin problems. Most skin problems are harmless, but even a minor one can become serious in people who have diabetes. A board-certified dermatologist can recognize skin problems due to diabetes and help you manage them.
Are all dermatologists board certified?
No. See what it takes to become board certified.
Images
Images 3, 7, 8, 9: Used with permission of the American Academy of Dermatology National Library of Dermatologic Teaching Slides.
Image 2 from DermNetNZ
Some images used with permission of Journal of the American Academy of Dermatology
Images 5, 6 and 10: Getty Images
References
Duff M, Demidova O, et al. “Cutaneous manifestations of diabetes mellitus.” Clinical Diabetes. 2015;33:40-8.
Kalus AA, Chien AJ, et al. “Diabetes mellitus and other endocrine disorders.” In: Wolff K, Goldsmith LA, et al. Fitzpatrick’s Dermatology in General Medicine (seventh edition). McGraw Hill Medical, New York, 2008:1461-70.
McKinley-Grant L, Warnick M, et al. “Cutaneous manifestations of systemic disease.” In: Kelly AP and Taylor S. Dermatology for Skin of Color. (first edition). The McGraw-Hill Companies, Inc. China, 2009:481-4.
Morgan AJ and Schwartz RA. “Diabetic dermopathy: A subtle sign with grave implications.” J Am Acad Dermatol. 2008;58:447-51.
Yosipovitch G, Loh KC, et al. “Medical pearl: Scleroderma-like skin changes in patients with diabetes mellitus.” J Am Acad Dermatol. 2003;48:109-11.
